Tertiary syphilis:
1. cardiovascular syphilis,
2. neurosyphilis (meningovascular syphilis, tabes dorsalis and general paralysis of the insane ).
3. “benign “tertiary syphilis.
After 5 years in 1/3rd of untreated patient
Cardiovascular syphilis
80% of cases of tertiary syphilis
Probably immune mediated
Endarteritis of the vaso vasorum leading to fibrosis of the media
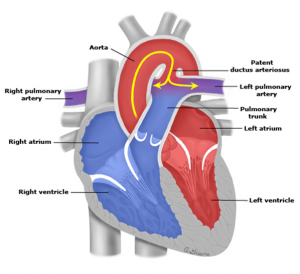
Increasing dilatation of the aortic root (leading to aortic incompetence) and arch (leading to an aneurysm).
Also, obstruction of the coronary artery ostia leading to ischaemia
Other causes of aortitis:
1. Giant cell arteritis (>50).
2. Takayasu’s arteritis (<50).
Both may involve the eye.
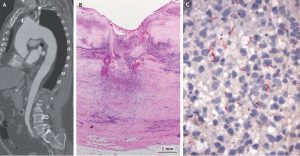
https://www.nejm.org/doi/full/10.1056/NEJMicm2110835
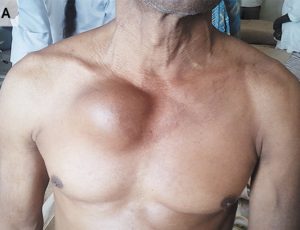
Avraham Z. Cooper, MD @AvrahamCooperMD
“Pulsatile chest swelling ➡️ HUGE aortic aneurysm from tertiary syphilis.”