Richard Smith of UnitedHealth and Adjunct Professor at IGHI, writes for the BMJ about our upcoming NCD event at the Royal Society on 4th October.
 I’m the minister of health in a poor country. Until last year I was a urologist. I was the president’s urologist and took out his prostate. To be honest, I don’t think it needed to come out, but he insisted. You don’t resist the president. He was delighted with the result and rewarded me by making me minister of health.
I’m the minister of health in a poor country. Until last year I was a urologist. I was the president’s urologist and took out his prostate. To be honest, I don’t think it needed to come out, but he insisted. You don’t resist the president. He was delighted with the result and rewarded me by making me minister of health.
It doesn’t feel like a reward. Everybody wants something from me, but I’m very low in the hierarchy. I don’t think that the minister of finance even knows who I am. When I talk about the dangers of tobacco, he smiles at me as if I’m a child who doesn’t know what he’s talking about.
What should be my priorities? That’s my big problem.
The president, who doesn’t now have a lot of time for me, tells me to reduce deaths, but not to spend any more money. He doesn’t seem to care how I reduce deaths (or even whether I do) so long as I don’t spend more money.
Other ministers mostly ignore me, unless their prostates are playing up. The minister of finance sends an official every month to make sure I’m keeping to my ludicrously small budget. The official never smiles.
Old colleagues from medical school tell me that the teaching hospital needs a lot more money. They want to expand neurosurgery, oncology, and the dialysis programme. They also want to start transplants and cardiac surgery for children. One of the professors in the medical school is trying to start a biobank and stem cell research. He talks about the unique genetic profile of our population.
Even though I’m a urologist, I feel that achieving the MDGs should be my priority. We’re not doing badly with reducing child deaths, although I know that in the remote area that I come from deaths are just as common as they were 10 years ago. The reductions have happened elsewhere.
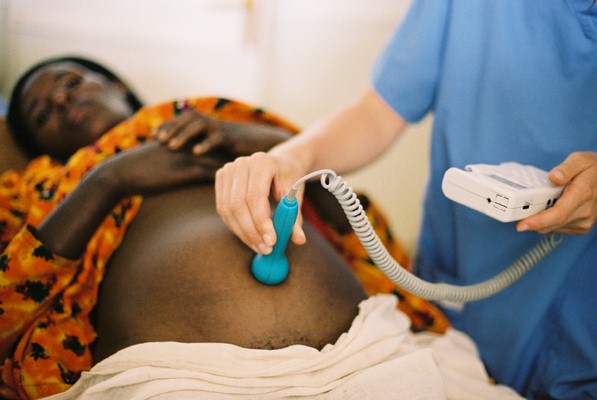 But we’re not doing well with reducing maternal deaths. All the religious leaders oppose family planning. I daren’t tell them (or anybody) that I’m an atheist. There are no obstetricians in the rural areas. They make too much money in the capital, and where would their children go to school if they were in the bush? But they won’t allow non-doctors to do Caesarean sections, and they won’t work with traditional birth attendants. They’re witchdoctors, they tell me. Whenever I try to persuade them to allow non-doctors to do Caesareans or to work with traditional birth attendants they run to the newspapers and talk about “second class care for second class people.”
But we’re not doing well with reducing maternal deaths. All the religious leaders oppose family planning. I daren’t tell them (or anybody) that I’m an atheist. There are no obstetricians in the rural areas. They make too much money in the capital, and where would their children go to school if they were in the bush? But they won’t allow non-doctors to do Caesarean sections, and they won’t work with traditional birth attendants. They’re witchdoctors, they tell me. Whenever I try to persuade them to allow non-doctors to do Caesareans or to work with traditional birth attendants they run to the newspapers and talk about “second class care for second class people.”
The clinics in rural areas are, I know, a disgrace. Patients go first to local healers. They try to avoid the clinics, partly because they are often asked to pay even though it’s supposed to be free, and partly because the staff are so rude to them. I don’t blame the staff. They are understandably demoralised, working with so many demands, little support, and so few drugs and supplies.
I’m just back from a trip to the UK. I did some postgraduate training in Edinburgh. I liked the city and even the food, but my God it was cold. While in Edinburgh I went to a meeting on global health. There was an ex-editor speaking, a loud mouthed guy with a Cockney accent, who talked about the need to act on non-communicable disease (NCD) in low income countries. He reminded me that we have signed up to the nine WHO targets on NCD, one of which is reducing deaths under 70 from NCD by 25% by 2025.
Should that be one of my priorities? In truth we don’t know how many people are dying, what they die of, or how old they are. We don’t have death certificates. I don’t know how many people are dying of NCD, but I know that there are still lots of children dying of diarrhoea and malaria. Nor do we have many people who know much about NCD. We’ve plenty of cardiologists in the capital, but they’re all run off their feet. And we don’t have a regular supply of drugs for hypertension.
At the same meeting a woman professor talked about stillbirths and argued that it was the most neglected of all global health problems. I’ve never thought about stillbirths.
While I was in the UK the Intergovernmental Panel on Climate Change published its report. I agree that this is the most important public health problem facing humankind, but the Americans, Europeans, and others in rich countries consuming lots of carbon need to recognise how the problem looks from my country. Most of our people are consuming less than 1% of the carbon consumed by people in rich countries, but we already suffering much more. Salt levels are increasing. Deserts are expanding. Our forests are disappearing because many people are still cooking with wood. We are doing what we can with developing solar power and giving people cookstoves, but we will have to consume more carbon in order to move our people out of extreme poverty. We need practical help, not preaching from the rich countries.
After the Edinburgh meeting I went to a meeting on global mental health at the Institute of Psychiatry in London. I couldn’t help noticing that the institute is in South London, very much the wrong side of the river, and that most of the people at the meeting were women, always a sign that the powerful are not that interested.
We have one psychiatrist in my country, and he’s retired. The awful truth, as one of the speakers said, is that in our country those with severe mental illness, usually schizophrenia, may be beaten, chained, starved, burnt, and sexually abused.
A man from WHO told us about the Global Mental Health Action Plan, which again we are signed up to. We have to reduce suicides by 10% by 2020, but again I don’t know how many suicides we have. I know that there are a lot, particularly among farmers, but nobody admits to it. We are also supposed to increase services for those with severe mental illness by 20% by 2020. This, I thought cynically, won’t be too hard because 20% more nothing is still nothing.
I’m still in London, staying with a friend. Later this week I’m going to a meeting at the Royal Society where a group of researchers from low and middle income countries are going to present their results and describe how they might help in countries like mine. I’ll be interested to see if they understand the pressures I’m under and have some practical way to help us.
This is, of course, from my imagination, but I did speak at the meeting in Edinburgh (and blogged on it), and there was a meeting at the Institute of Psychiatry last week that I attended briefly. There is also a meeting on Friday 4 October at the Royal Society, with presentations of the results of five years of research into NCD from the directors of 11 centres from low and middle income countries. Admission to the meeting is free, and you are invited to attend. Come and find out if the imaginary minister of health will learn something useful.
Competing interest: RS is an employee of UnitedHealth, which, together with the National Heart, Lung, and Blood Institute, has funded the 11 centres. He is also an adjunct professor at the Imperial College Institute of Global Health Innovation and a trustee of C3 Collaborating for Health, two organisations that are hosting and organising the meeting at the Royal Society.