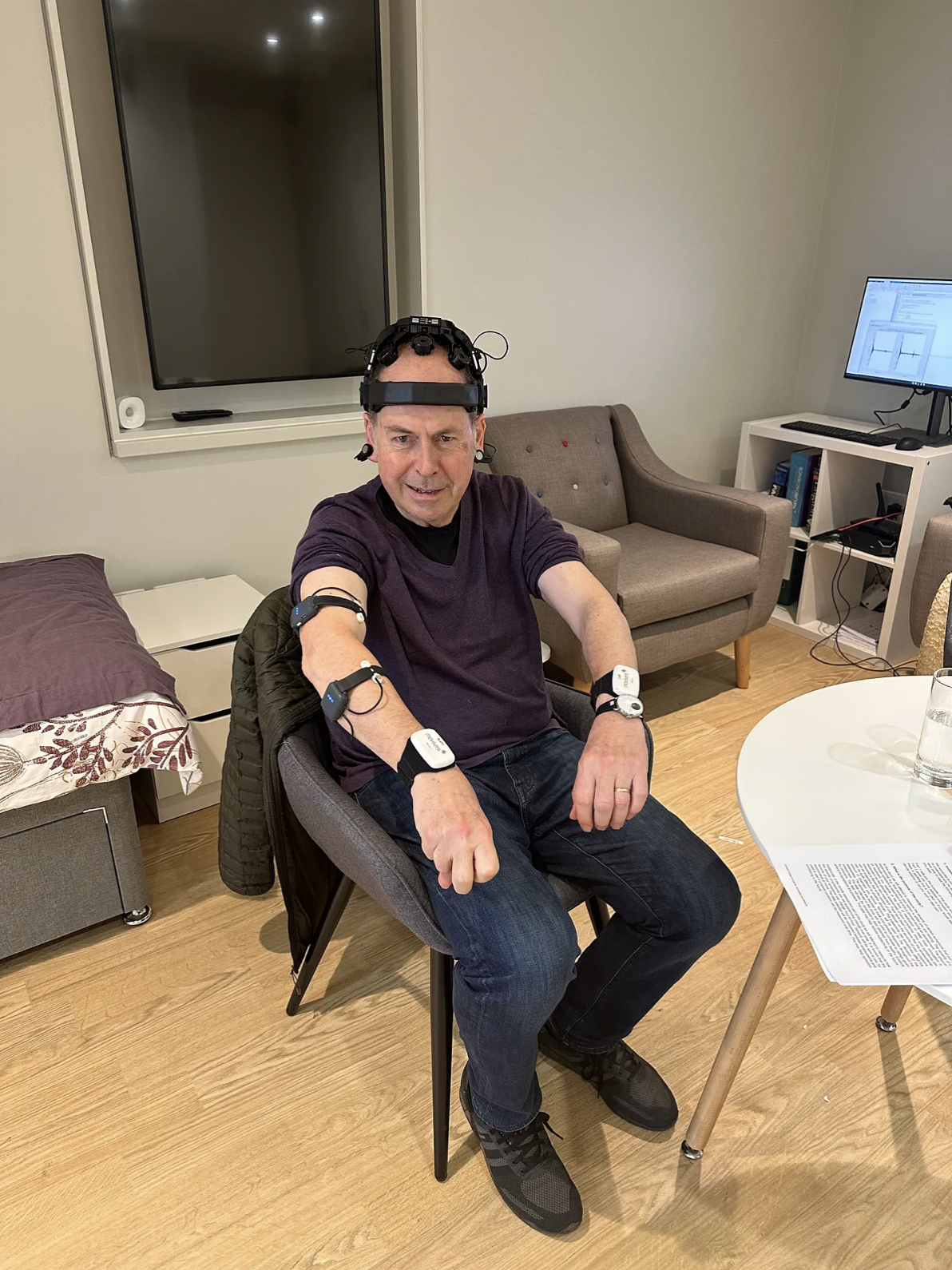
Despite major progress in treatment and prevention, being diagnosed with HIV can have a big emotional impact on individuals. People with HIV have higher rates of mental health problems than those seen in the general population. One reason for this may be HIV-related stigma, explains Professor Alan Winston from the Department of Infectious Disease.
Since the late 1990s, I have been treating people living with HIV and been involved in HIV clinical research. Many things we read about HIV are success stories, and quite rightly we should celebrate these tremendous scientific and medical advances. Life expectancy for someone with HIV is now similar to that of the general population. Antiretroviral therapy generally has manageable side effects and for most individuals, does not incur that many tablets per day. Indeed, many HIV treatments involve taking only one tablet per day. So, why then do so many people with HIV suffer from depression, other mental health conditions, and a poorer quality of life?
Experience in clinic
Most people living with HIV, once on a stable treatment, will attend their treatment centre twice per year. Often appointments rotate between a consultant or medical doctor once per year and a nurse specialist on the other occasion. As we can’t cure HIV, our patients attend for life, and we get to know them very well. At consultations, in addition to routine monitoring, we ask people how they are keeping. What stands out are the number of individuals who report symptoms of depression and other mental health conditions such as anxiety. Whilst many of us suffer from mental health complaints, the burden of these complaints in people living with HIV is very high. Thankfully, we do have help in clinic and have a specific clinic run by a psychiatry nurse specialist we can refer patients to.
 Kelly Gleason introduces a guide,
Kelly Gleason introduces a guide,